Article originally published by Neuronews.
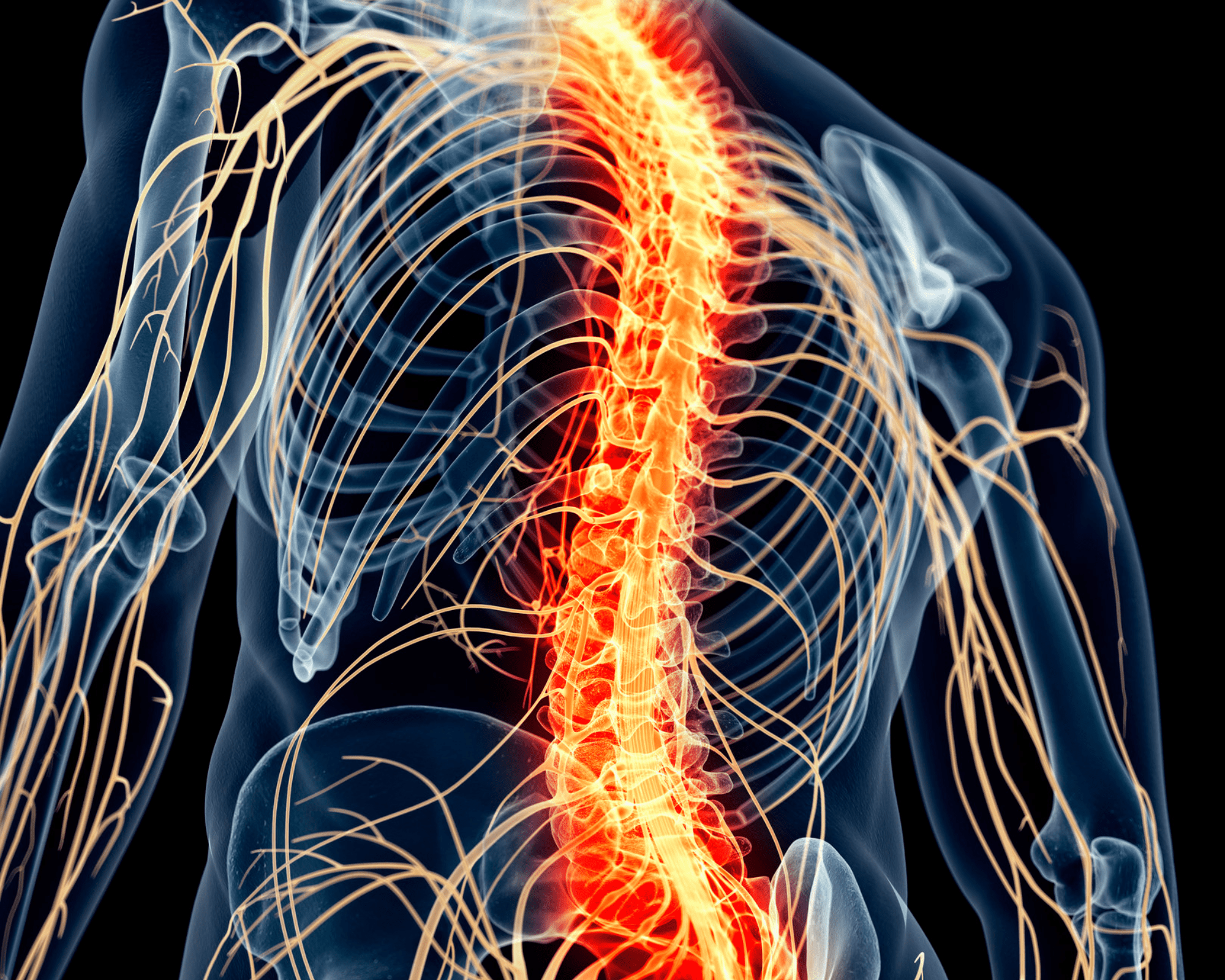
A recently published Cochrane review has concluded that the clinical benefits of spinal cord stimulation (SCS) do not outweigh the risks and costs associated with the approach in patients with low back pain—leading researchers to claim that “there is clearly a problem here that should be of concern to regulators”.
Writing in the Cochrane Database of Systematic Reviews, the researchers involved state that SCS therapy does not provide long-term relief or sustained benefits based on the current evidence, and may cause harm.
“Spinal cord stimulation is invasive and has a great financial cost to people who choose surgery as a last resort to alleviate their pain,” said lead researcher Adrian Traeger (Sydney Musculoskeletal Health, Sydney, Australia). “Our review found that the long-term benefits and harms are essentially unknown.
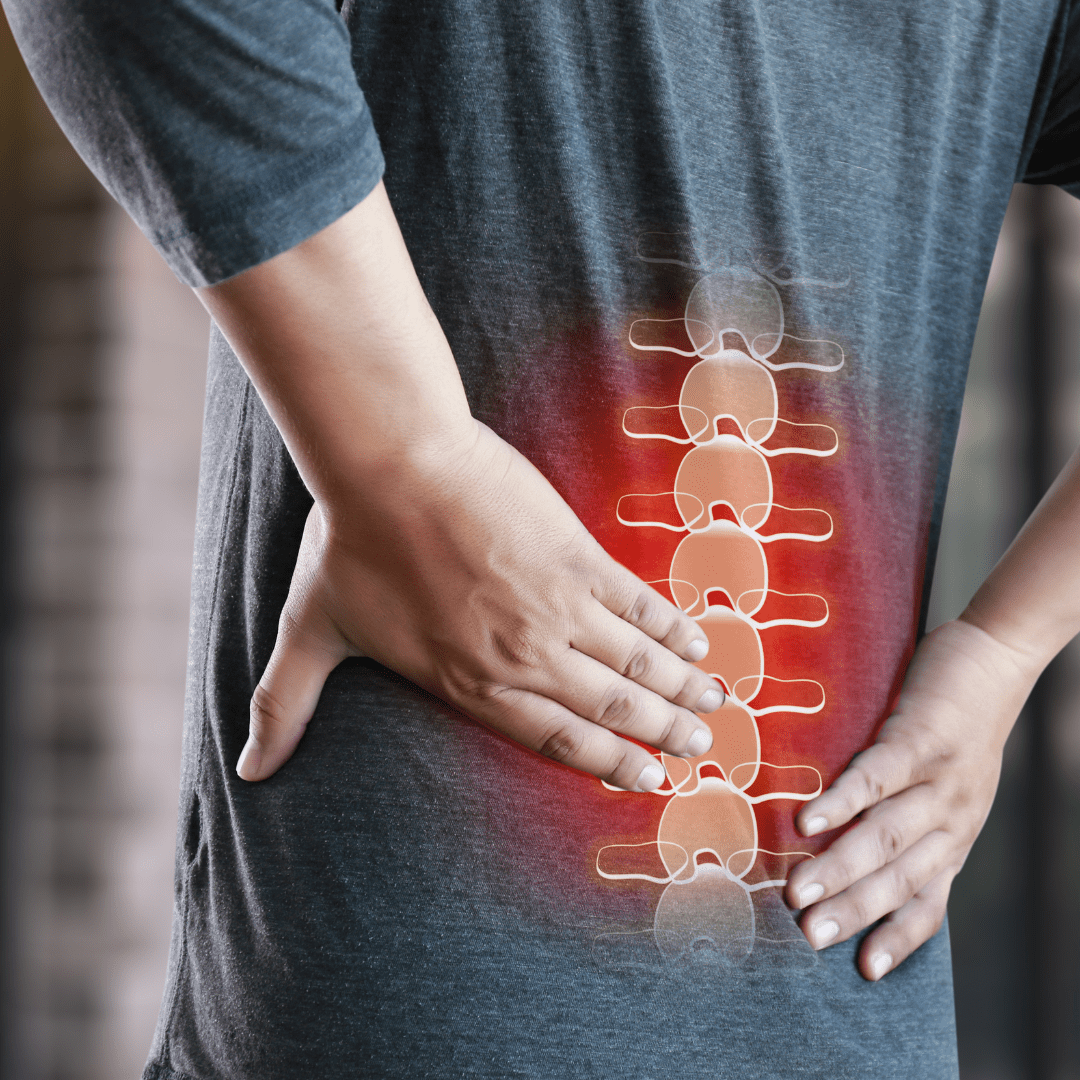
Low back pain is one of the leading causes of disability worldwide.
Our findings further emphasise the urgent need to review funding arrangements for chronic pain care to help patients in their search for relief. There are evidence-based physical and psychological therapies for back pain; ensuring access to these is essential.”
New evidence on SCS
The present study reviewed published clinical data on SCS, including randomised controlled trials. The researchers analysed the results of 13 trials, looking at data from a total of 699 participants, comparing SCS treatment with placebo or no treatment for low back pain. They elected to do this via a Cochrane review given these approaches use “robust methodologies to combine evidence from multiple sources, reducing the impact of bias and random error that can make individual studies less reliable”.
The review concluded that SCS is “no better than a placebo” for treating low back pain, with “probably little-to-no benefit” for people with low back pain nor improvement in their quality of life. The researchers add that there were “little-to-no clinical data regarding the long-term effectiveness of SCS”, and that they found data detailing adverse side-effects associated with SCS surgery were “poorly documented overall”, preventing them from conclusively determining the level of risk involved.
Potential sources of harm from SCS could include nerve damage, infection, and the electrical leads moving—all of which may mean repeated surgeries are required, the researchers also detail.
The review team claims to have found multiple gaps in the existing clinical data. For example, there were no studies that investigated the long-term (>12 months) impact of SCS on low back pain, with the longest being a single six-month trial. The majority of clinical trials “only looked at the immediate impact of the device”, which is a time frame of less than one month, the researchers note.
The big picture
According to a news release from the University of Sydney (Sydney, Australia), these review findings have been submitted to the Federal Department of Health and Aged Care prosthesis list review taskforce. In Australia, the long-term safety and performance of SCS devices is also currently being re-assessed by the country’s Therapeutic Goods Administration (TGA).
The review team further provided a list of recommendations, including that future clinical trials of SCS should be conducted across at least 12 months; clearly document the number of people who experience adverse events; and make comparisons with other pain treatment options.
“Our review found that the clinical benefit of adding spinal cord stimulation to treat low back pain remains unknown,” said Chris Maher, co-director of Sydney Musculoskeletal Health. “When coupled with the reality that these devices are very expensive and often break down, there is clearly a problem here that should be of concern to regulators.”
A separate Cochrane review led by investigators from the UK and published in late-2021 examined the effect of SCS therapy versus placebo in people with chronic pain and—similarly to the present study—concluded that there was a lack of evidence to suggest long-term benefits.